Conditions · Menopause transition
A decade of physiology, almost no monitoring.
The menopause transition spans years and overlaps with rising cardiometabolic risk — yet most women navigate it without longitudinal biomarker data. The Q-Pad enables a longitudinal endocrine record at home.
The condition
A multi-year reproductive-aging window.
The menopause transition is the multi-year reproductive-aging window leading to the final menstrual period (FMP), defined retrospectively after twelve months of amenorrhoea. The Stages of Reproductive Aging Workshop (STRAW+10) divides the transition into early and late perimenopause based on cycle variability and hormonal markers; perimenopause typically begins in the mid-40s and lasts 4–8 years [1]. Symptom burden — vasomotor, sleep, mood, cognition, urogenital, cardiometabolic — is substantial.
Standard of care
Diagnosed clinically, monitored rarely.
Menopause is diagnosed clinically. Hormonal testing is rarely indicated in routine perimenopausal care because levels fluctuate cycle-to-cycle, and a single venous draw is uninformative [2]. As a result, most women navigate the transition without longitudinal biomarker data — even though it spans a decade and overlaps with rising cardiometabolic risk.
Why menstrual blood
Multi-cycle hormonal data, at home.
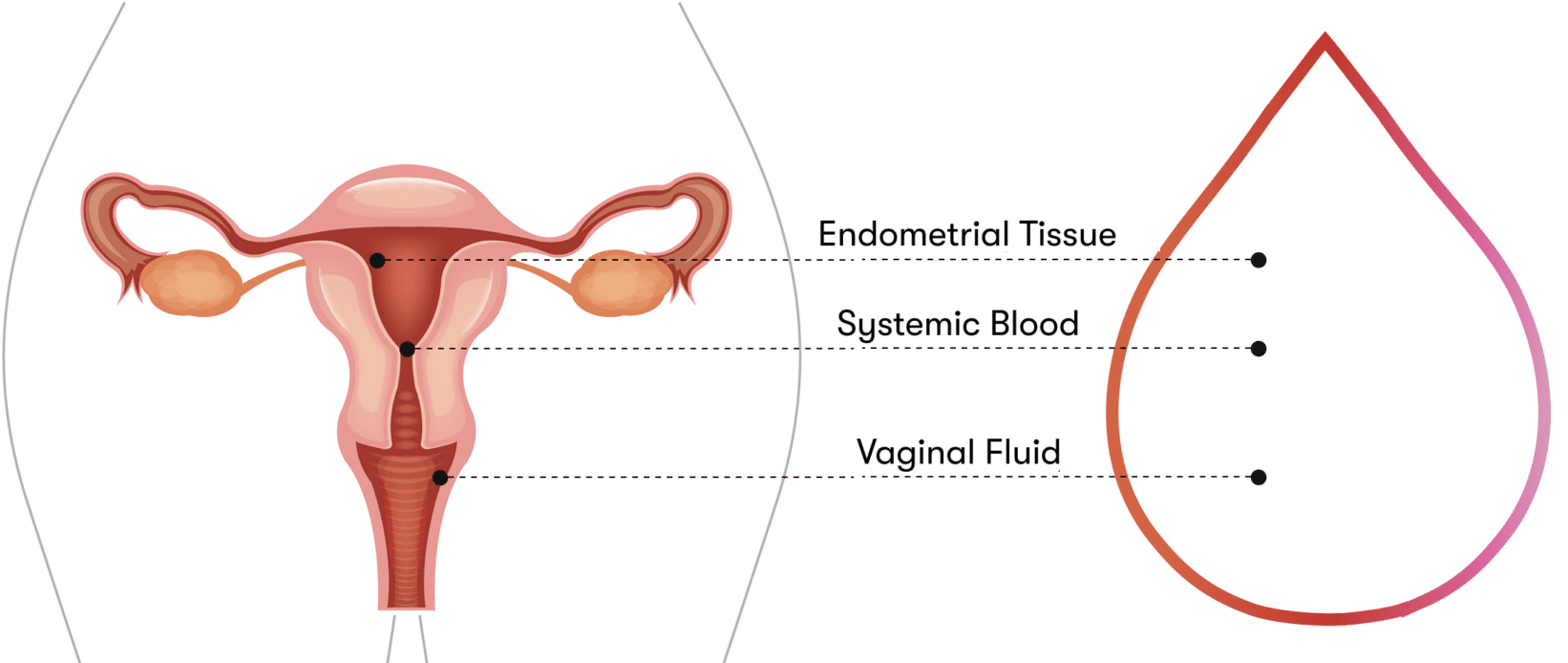
The Q-Pad's recurring at-home collection format is what hormonal monitoring across the transition has lacked. Validated correlations between menstrual blood and venous draws for FSH, LH, estradiol, AMH, and TSH support multi-cycle monitoring of the very analytes that change through perimenopause [3]. A second sample type — endometrial-derived signal — opens additional research questions about uterine aging that aren't accessible from peripheral blood.
Qvin's role
Wellcome Leap–funded perimenopause work.
Menopause is one of Qvin's most active programs, supported by a Wellcome Leap–funded collaboration with the University of Exeter exploring perimenopause biomarkers. The clinical end-point is a longitudinal home-collection panel that helps clinicians and patients navigate the transition with evidence rather than guesswork.
References
Sources
- Harlow SD, Gass M, Hall JE, et al. Executive summary of the Stages of Reproductive Aging Workshop +10. Journal of Clinical Endocrinology & Metabolism 97(4):1159–1168, 2012. doi.org/10.1210/jc.2011-3362.
- National Institute for Health and Care Excellence (NICE). Menopause: diagnosis and management (NG23). NICE guideline, 2015 (updated). nice.org.uk/guidance/ng23.
- Naseri S, Rosenberg-Hasson Y, Maecker HT, Avrutsky MI, Park CL. Demonstration of menstrual blood as a viable source for screening and diagnostic clinical applications: a pilot study. BMC Women's Health, 2023. bmcwomenshealth.biomedcentral.com.
Other conditions