Conditions · Endometrial cancer
A gynecologic cancer with no screening test.
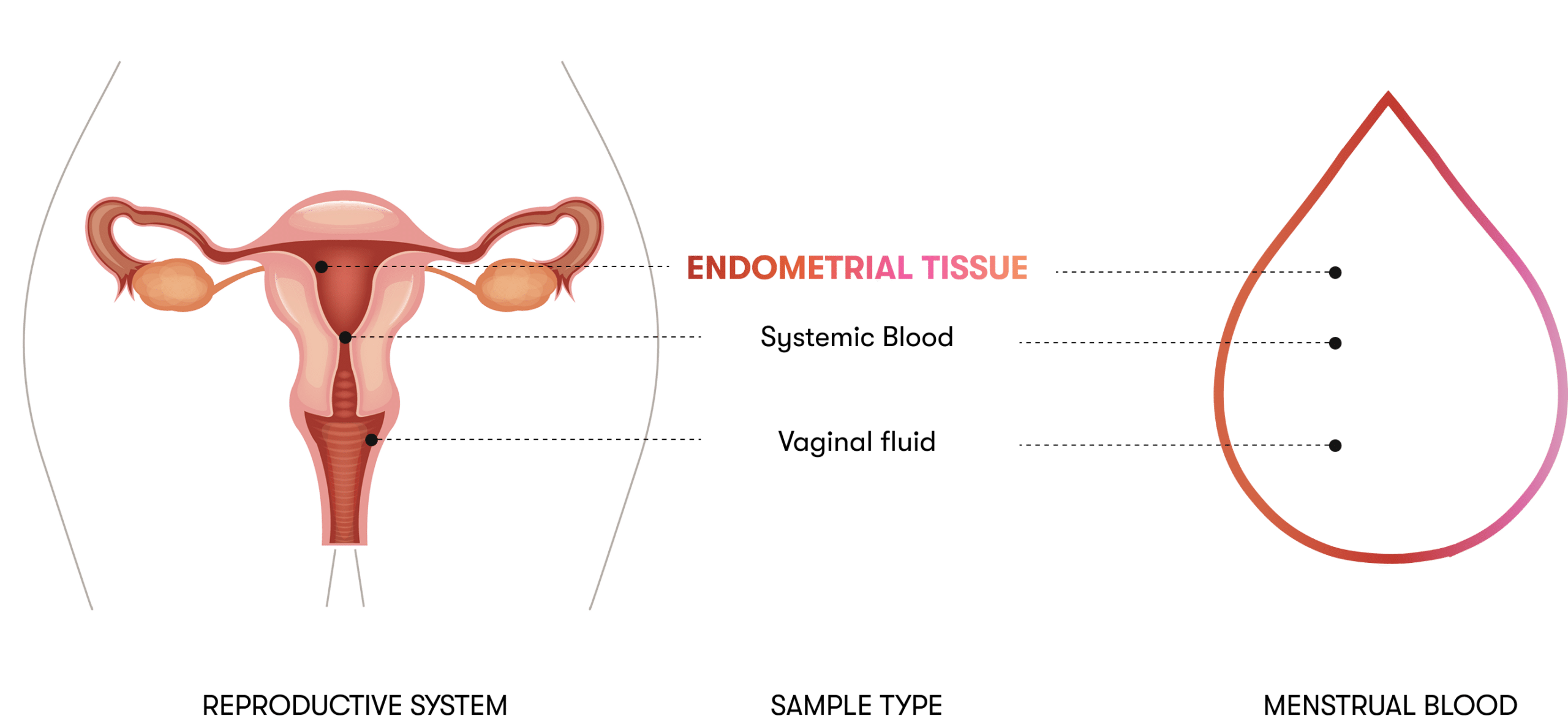
Endometrial cancer is the most common gynecologic malignancy in high-income countries. Menstrual blood carries shed endometrial tissue — the tissue of origin for the disease.
The condition
Most common gynecologic malignancy in high-income markets.
Endometrial cancer is the most common gynecologic malignancy in high-income countries, with rising incidence and mortality driven in part by population-level increases in obesity and metabolic disease [1]. Most cases are diagnosed at an early stage when symptomatic (post-menopausal bleeding, abnormal uterine bleeding), but younger pre-menopausal patients are increasingly affected, and there is no general-population screening test.
Standard of care
Symptom-driven workup, no screening analogue.
Workup is symptom-driven: transvaginal ultrasound followed by endometrial biopsy or hysteroscopy in patients with concerning bleeding. There is no analogue of cervical screening for the endometrium, and the absence of a screening test contributes to delayed diagnosis in younger and obese patients, who often present after months of abnormal bleeding.
Why menstrual blood
The tissue of origin, in the sample.
Menstrual blood contains shed endometrial tissue from the patient's own uterine cavity — the tissue of origin for endometrial cancer. Recent research using uterine lavage and intra-uterine sampling demonstrates that tumour-derived genomic signal is detectable in the endometrial cavity, sometimes before symptomatic presentation [2]. A non-invasive substitute for that sampling, in an at-home collection format, is the natural translation question.
Qvin's role
A discovery-track program.
Endometrial cancer is a discovery-track program. Work is institution-collaborated and early-stage; the goal is a Q-Pad-compatible aid-in-diagnosis or screening assay for at-risk groups (post-menopausal bleeding, obese pre-menopausal women, hereditary cancer syndromes such as Lynch).
References
Sources
- Crosbie EJ, Kitson SJ, McAlpine JN, Mukhopadhyay A, Powell ME, Singh N. Endometrial cancer. The Lancet 399(10333):1412–1428, 2022. doi.org/10.1016/S0140-6736(22)00323-3.
- Casas-Arozamena C, Díaz E, Moiola CP, et al. Genomic profiling of uterine aspirates and ctDNA as a tool for endometrial cancer detection and characterization. Cancers 12(9):2554, 2020. doi.org/10.3390/cancers12092554.
Other conditions